
My morning ends and I have completed a weekly food shop. When I first arrived at the supermarket I was told that the first hour was reserved for people aged 70 and older, later as I stood in the queue I noticed an invite to National Health Service (NHS) workers to go straight to the front, both of course very good measures for these groups. There is no doubt that the NHS are at the forefront of responding to the COVID19 pandemic and best placed to provide treatment. ‘Stay home, protect the NHS and save lives’ goes the simple, enormously successful slogan. Yet why no invite for social care staff? The answer is a complex one. Here are some of the reasons, all of which are interrelated.
Lack of understanding: Social care isn’t well understood by the public; in a recent poll half the respondents thought that it was free at the point of need and over half of those polled thought that social care was provided by the NHS. The latter is likely to stem from a misunderstanding about what social care does; certainly the status afforded to health workers is not extended to social care.
Low pay and low status: A striking aspect of the present crisis is that many keyworkers are low pay and low status: street cleaners; bin collectors; supermarket workers and social care workers. The view of pay boards is that the skills needed by the largely female workforce of care workers are akin to those of a the largely male bin collector workforce. The low status is systemic; consider how the rhetoric focuses on supporting the care sector so that we can protect the NHS; consider the way patients were discharged from hospitals to care homes without routine testing for COVID19; look at how the guidance on personal protective equipment in social care took weeks to arrive at the present more precautionary approach; look at how long it took for personal protective equipment to reach care homes; look at how deaths from COVID19 within care homes weren’t included in the daily tally of sorrow until late April; then look at the catastrophic toll wreaked by the virus on care homes.
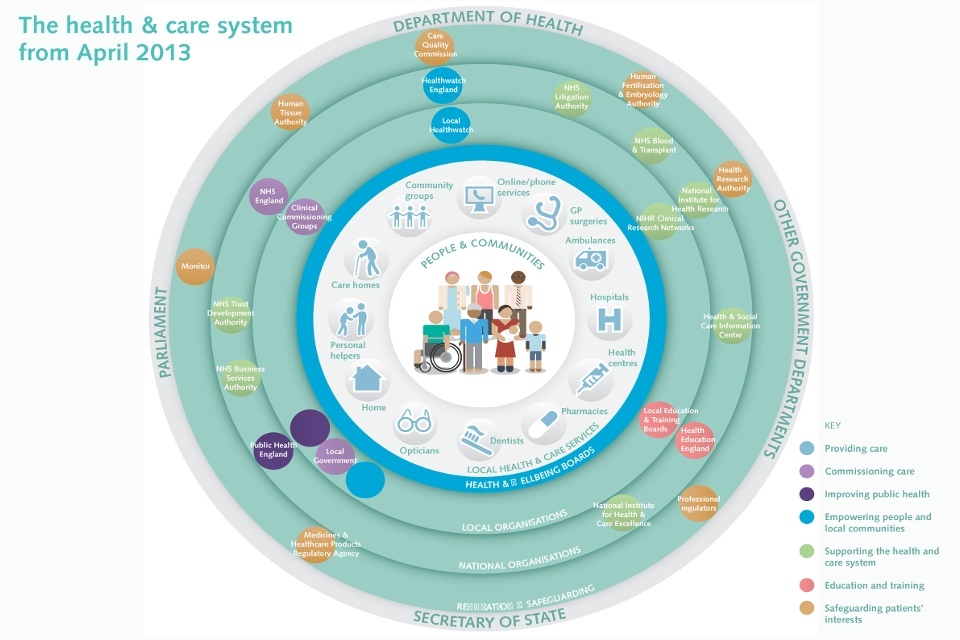
Social care is a complex, largely private market. The reason for this stems back to the Community Care Act (1990) which required local authorities to meet social care needs through the private sector. Now around 90% of provision is within the private and voluntary sector, with an emerging ‘personal assistant’ workforce. The illustration below from 2013 shows the complex inter-relationship between the stakeholders in the social care world. Since then ‘social care’ has been added to the Department of Health, otherwise the stakeholder map largely reflects the present situation. Consequently creating clarity, continuity and consistency is difficult and the voice of social care is very much weaker than that of the NHS.
Lack of visibility and brand. With some justification the NHS claim their iconic, authoritative, calming, clean blue and white brand “is one of the most cherished and recognised brands in the world. When applied correctly and consistently, it evokes exceptionally high levels of trust and reassurance.” There is no equivalent for social care and at last the Health and Social Care Secretary has decided that enough is enough and help is at hand with the reviving of the care badge. Looking like a rejected 90’s website banner the care badge was launched to national indifference in June 2019.

Years of inaction. Years of austerity have pulled social care to its knees. It’s likely that if the local authority is funding your place in a care home then your fellow self-funding residents are cross subsiding your care. The government know that social care is in trouble and have been promising a green paper for years.
Until the problems facing social care are properly addressed the sector will remain low pay, low status and our loved ones will pay with their lives. When the coronavirus crisis passes let’s not return to business as usual, let’s do something better.